The second trimester of pregnancy is from week 13 to week 28 – roughly months four, five and six.
A second trimester sonogram is usually performed between weeks 18-20.

The Scan
Before you begin your exam make sure your gel is warm and your patient is comfortable.
When I a scan I like to begin in the lower uterine segment. This allows you to visualize the cervix and check fetal position.
Vertex or Cephalic – Fetal head is the presenting part.
Transverse – Fetus is laying horizontally in the uterus. Head may be to the mothers right or left.
Breech – Fetal rump or legs are the presenting part.

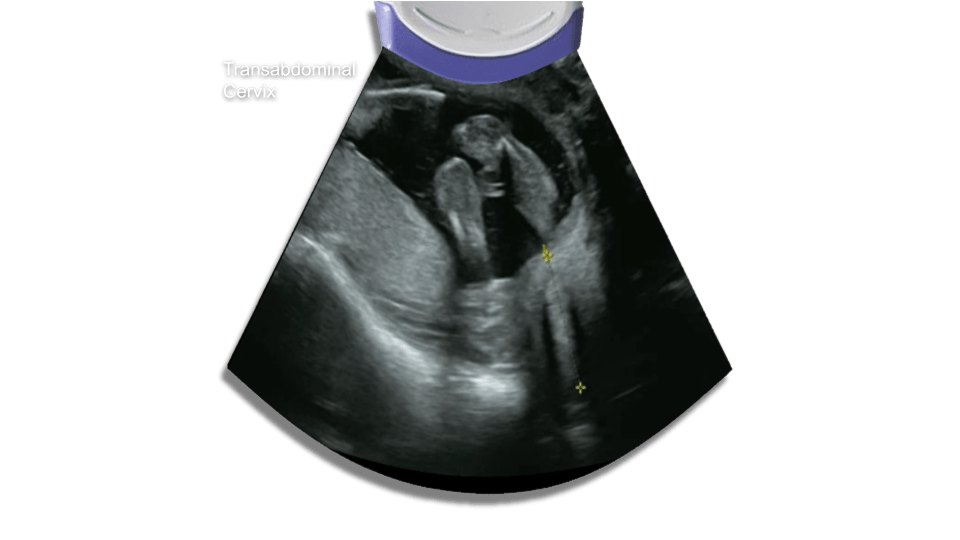
Cervix
The average length of the cervix is 3.5 cm. The cutoff usually used is 2.5 cm. If there is any cervical shortening or funneling (amniotic membranes bulging into the cervix) you may obtain a transvaginal ultrasound to confirm.
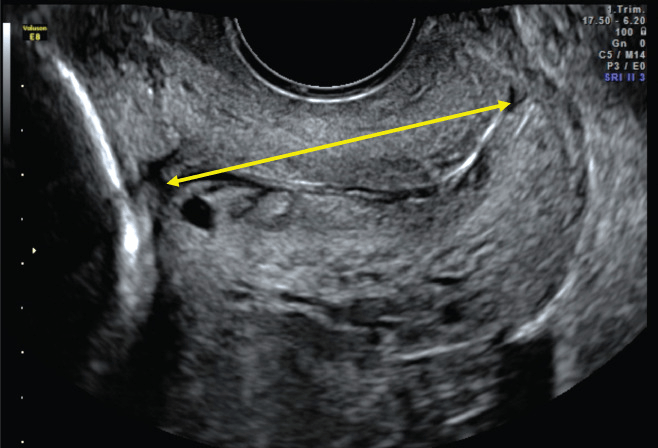
Potential pitfalls for transabominal approach:
Overfilled bladder masking cervical incompetence, also an underfilled bladder might make the cervix hard to image.
Anatomy
Proceed to check the fetus in a head to toe fashion. Begin with the head, you’ll take measurements like the biparietal diameter (BPD), head circumference (HC) and survey the intracranial anatomy like the cerebellum, posterior fossa and lateral ventricle to name a few.
Head and Neck

Biparietal Diameter
Fetal Biometry
There are 4 basic measurements for fetal weight and age estimation, biparietal diameter, head circumference, abdominal circumference and femur length.
BPD – Biparietal diameter of the fetal head is obtained in a transverse position at the midbrain
Landmarks interhemispheric fissure (falx), cavum setpum pellucidum, and thalamus.
A normocephalic head is oval and should be symmetrical. Measure from the outer parietal bone to the inner parietal bone.
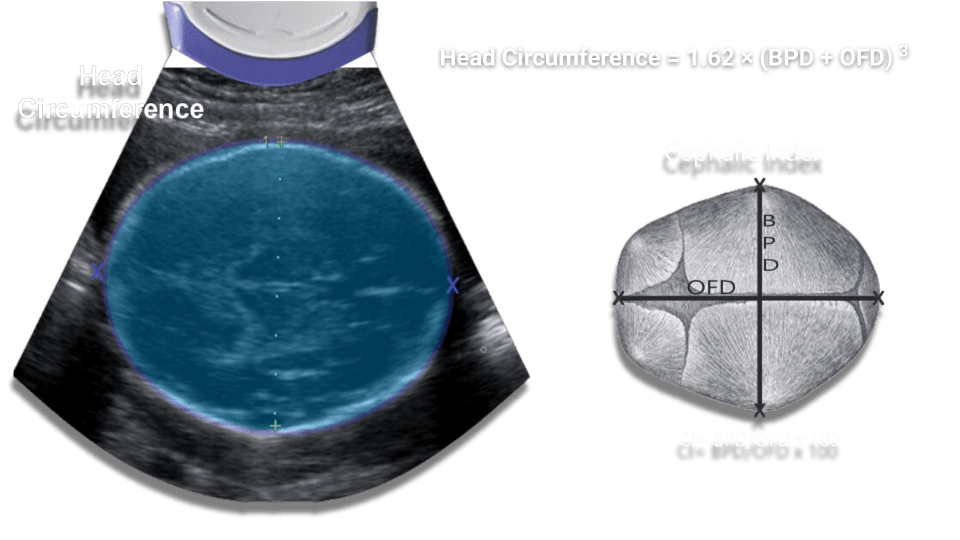
Head Circumference
HC- The head circumference is taken at the same level as the BPD. Place the calipers from anterior to posterior using the ellipse to cover the outer margins.
dolicocephaly (long anterior to posterior lenght) and brachycephaly (short anterior to posterior length) can give you inaccurate dates.
Survey the intracranial anatomy for normal landmarks.
Image the orbits, document eye distance, eye movement including blinking.

Imaging the head and neck can rule out things like hydrocephalus, agenesis of the corpus callosum, holoprosencephaly, cerebellar issues like banana sign along with lemon sign which can be indicative of spina bifida. Also cleft lip/ palate. Perform measurement of the nasal bone which if absent can be a marker for Trisomy 21.
Neck
Descend to the neck, check and measure the nuchal fold or nuchal translucency. There are two measurements you can take.
One being the nuchal translucency, which is measured earlier (between 11-14 weeks) in pregnancy at the end of the first trimester for which there is a lower threshold for increased diameter or the nuchal fold, which is measured towards the end of the second trimester.

You can also scan the neck to check for nuchal cord. This is when the cord is wrapped around the neck and can potentially cause asphyxiation.

Also check for cystic hygromas. Which are fluid-filled sacs that occur most commonly on the head or neck of a fetus. They are a result of blockages in the lymphatic system.

Chest
Scanning the chest look at lungs and check the echogenicity, r/o pleural effusion, cystic adenomatoid malformation, look at diaphragm and check for diaphragmatic hernia. Check diaphragmatic movement for breathing.
Heart, stomach and bladder view can rule situs inversus.
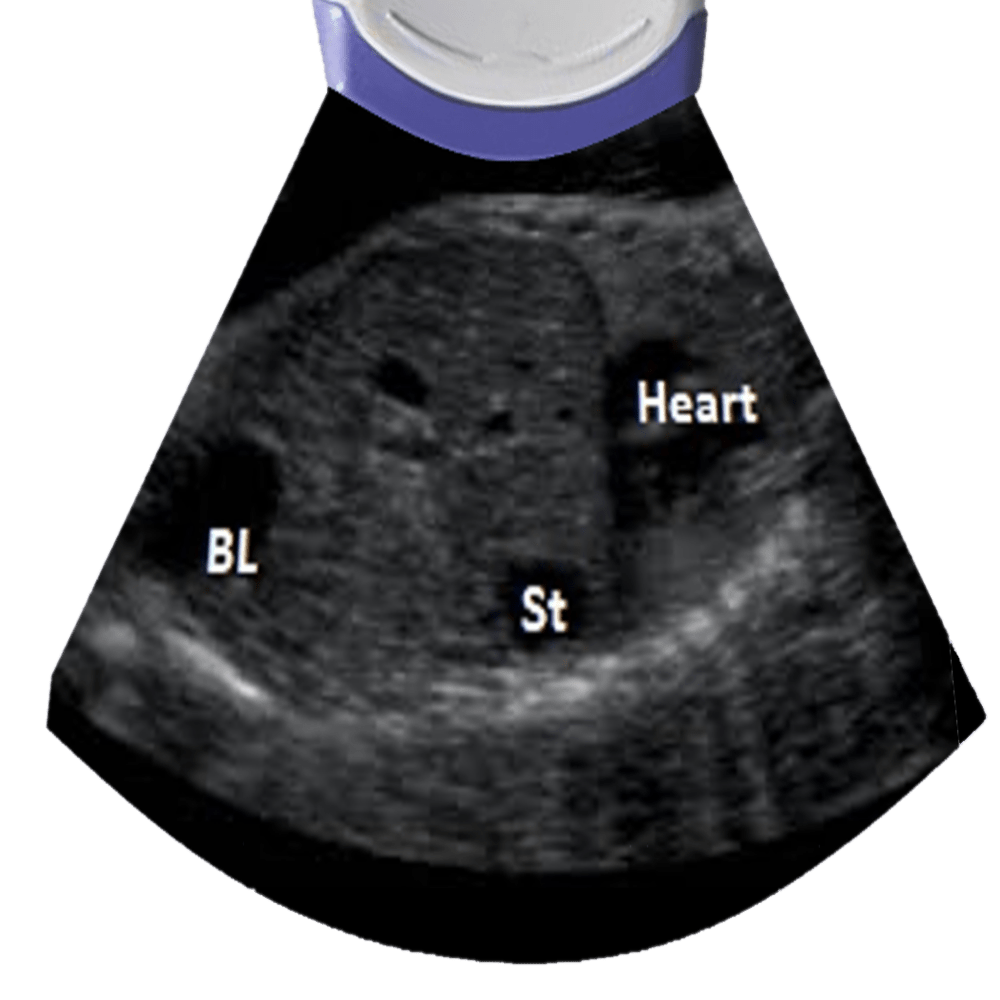
Heart size relation to chest (hear takes up 1/3 of the chest with the apex pointing to the left).
Four chamber view, also asses the lung parenchyma.
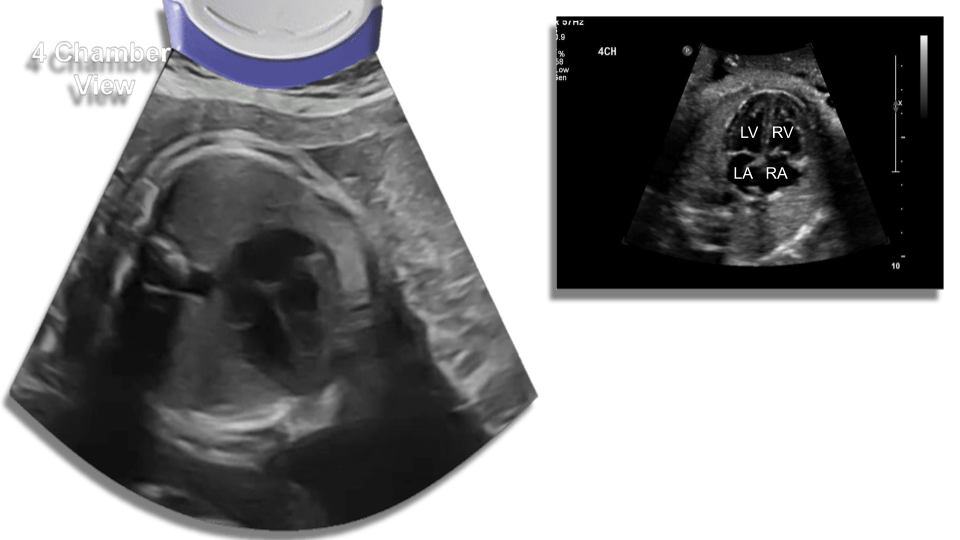
Aortic Arch

Perform cardiac m-mode for fetal heart rate look out for arrhythmias, tachycardia, bradycardia or lack of cardiac activity (fetal demise.)

Upper extremities
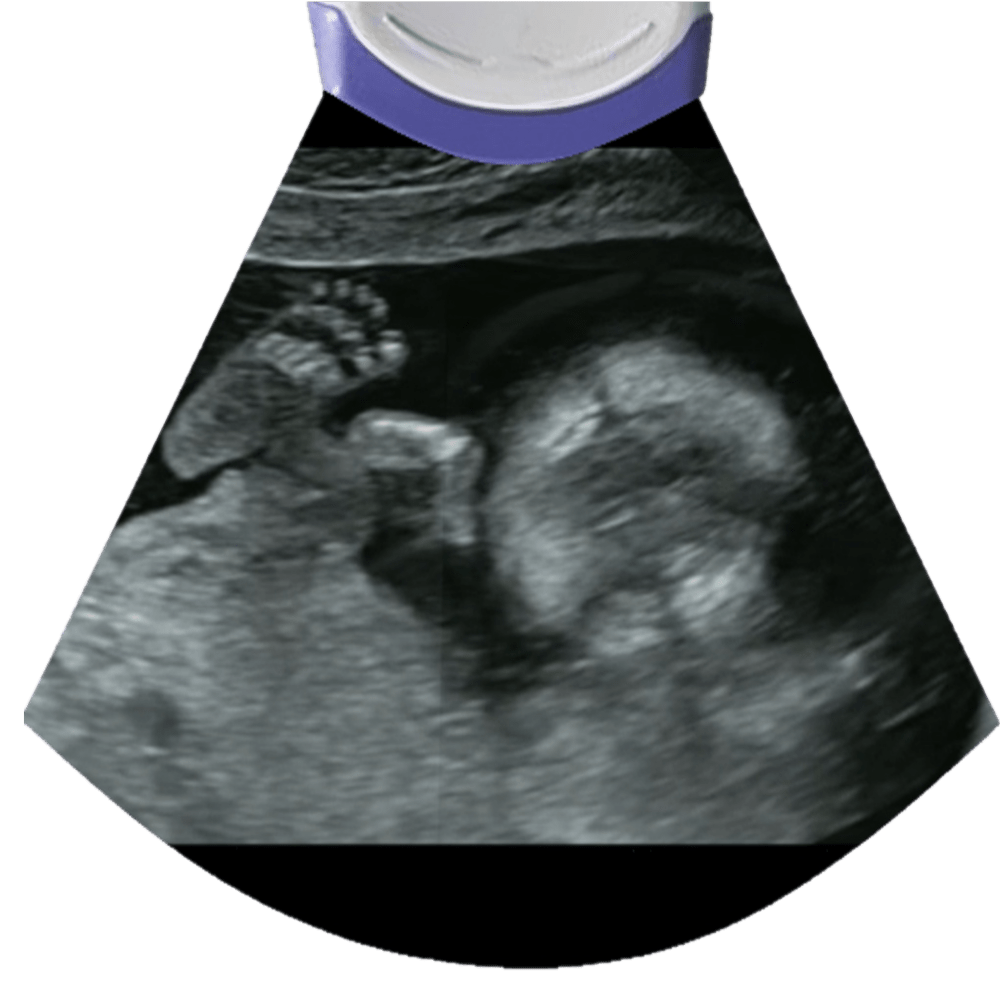
Scan both arms, confirm the presence of bilateral humeri, radius and ulna. Check for asymmetries or size discrepancies that can be related to skeletal dysplasias.
Check the number of fingers.

Spine
Image the spine in sagittal, transverse and coronal.

Abdomen
AC – abdominal circumference should be taken from a transverse abdomen above the umbilical cord insertion at the level of the stomach, liver and the umbilical portion of the portal vein.
Measure the outer margin.

The liver is largest internal organ, asses the hepatic vasculature and check for lesions like hemangiomas, cysts and calcifications. The gallbladder can sometimes be seen. Occasionally fetal gallstones can be seen (not very common but possible). Also check for abdominal wall defects like omphalocele and gastroschisis.
Kidneys
Asses the kidneys for location, echogenicity. Evaluate for hydronephrosis, renal agenesis, ectopia, cysts or solid masses. Image the kidneys in sagittal, coronal and transverse planes.

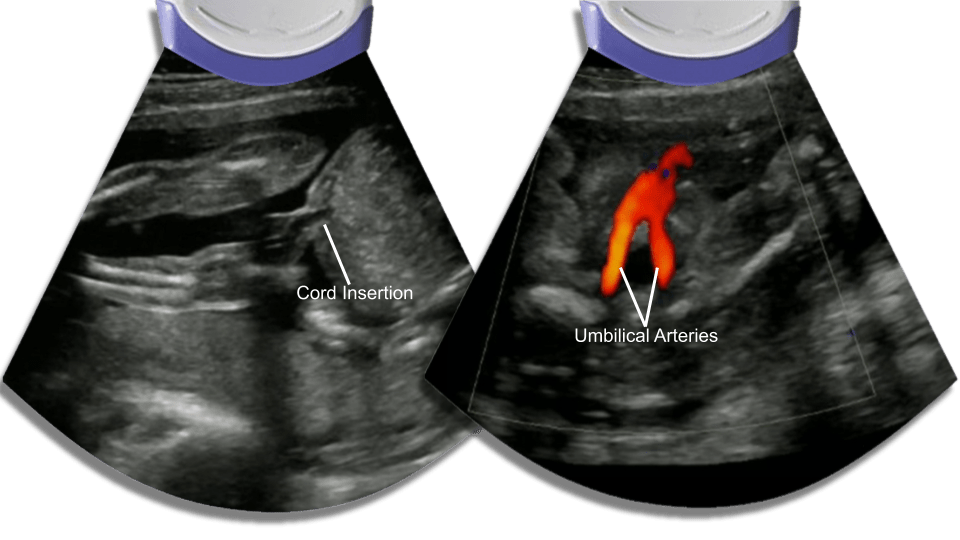
Cord Insertion
The normal umbilical cord has 3 vessels, two arteries and one vein. The umbilical arteries go down pass the bladder into the bilateral iliac arteries and the umbilical vein travels up into the liver. good place to rule out omphalocele and and bladder extrophy.
Bladder
The bladder could be empty, it fills every 30 to 45 minutes or so. look for bladder extrophy, keyhole bladder which indicate posterior urethral valves.

Here you can determine the gender of the fetus.

Lower Extremities
Femur length
The femur can be seen in the bilateral thighs of the fetus. The hyperechoic portion is the femoral diaphysis. Measurement is from the greater trochanter to the femoral condyles.
Discrepancies or asymmetries can be used to indicate skeletal dysplasias or growth restriction.

Asses the tibia and fibula, same as upper extremities check for signs of skeletal dysplasias.
Make sure there are 5 toes in each foot, look for things like club foot, rocker bottom foot and sandal gap.
Placenta
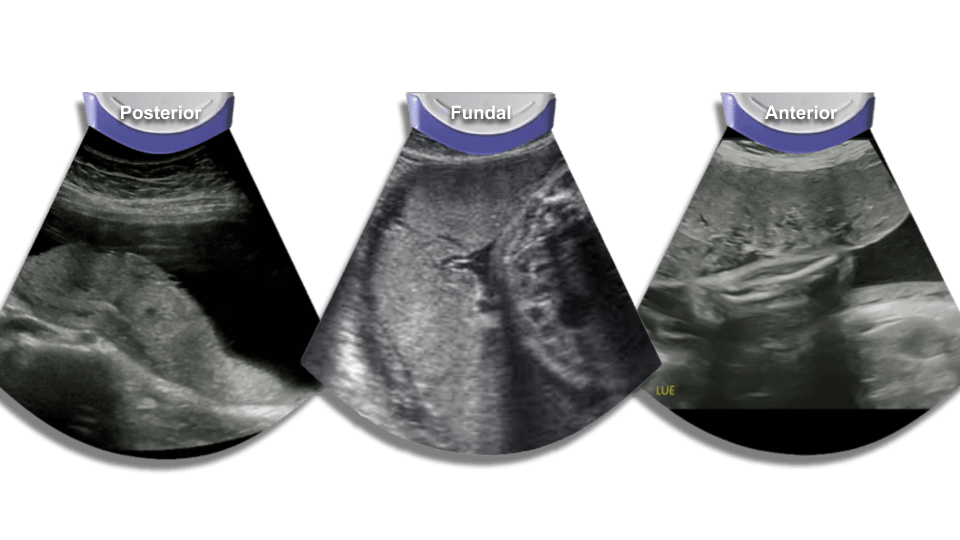
Check for position (fundal, posterior, anterior, previa). Check the cord insertion into the placenta as well.
Placenta previa

Placenta previa is a condition in which the placental tissue lies abnormally close to the internal cervical os. The 4 generally recognized subtypes are
- Complete – the placenta is covering the entirety of the internal os
- Partial – the placenta is covering a portion of the internal os
- Marginal, in which the placental tissue abuts but does not cover the internal cervical os; and
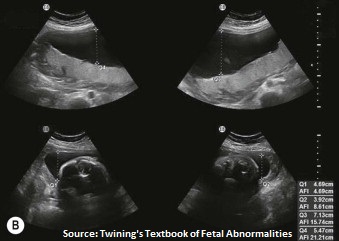
Amniotic Fluid
The amniotic fluid can be anechoic or have low level echoes (vernix). In order to obtaion the amniotic fluid index AFI, divide uterus into four quadrants via the linea alba and umbilicus , measure largest vertical pocket in each quadrant excluding cord.
An abundance of fluid is termed polyhydramnios, too little fluid is oligohydramnios

This post is a brief overview here I’m linking to a video with more in depth analysis of the anatomy and some pathology.
Sources:
Hadlock, Frank P., et al., “Estimation of Fetal Weight with the Use of Head, Body, and Femur Measurements—A Prospective Study.” American Journal of Obstetrics and Gynecology, vol. 151, no. 3, 1985, pp. 333–337., doi:10.1016/0002-9378(85)90298-4.
Hagen-Ansert, Sandra L. Textbook of Diagnostic Ultrasonography. Mosby Elsevier, 2006.




Best one
LikeLiked by 1 person
Thanks!
LikeLike
I greatly appreciate all your hard work. I have referenced your site many times. Many thanks.
LikeLike
Happy to hear that!
LikeLike
Thank you very much!!
LikeLike
[…] scan is done between 18 and 22 weeks of pregnancy5. It’s a vital part of prenatal care6. Your doctor uses high-tech imaging to check on your baby’s brain, heart, kidneys, and more4. […]
LikeLike