Veins are blood vessels that carry deoxygenated blood toward the heart (with the exception of the pulmonary and portal veins which carry oxygen rich blood to the left atrium and liver respectively). Veins and arteries are made up of the same 3 layers
- tunica intima: Inner most layers comprised of endothelial cells
- tunica media: middle layer comprised of smooth muscle
- tunica adventitia/externa: external layer made up of fibrous connective tissue.
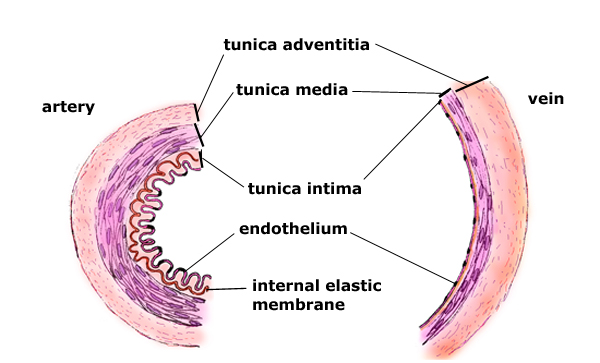
Another difference between the vein and artery is the medial layer, with the arteries tunica media being thicker than the veins.
Veins have lower internal pressure than arteries, they also have valves. Forward blood flow in the artery is maintained by the heart, which acts as a pump propelling the blood onward with each beat. In the veins, especially in the extremities, the limb muscles act as this pump. With each step we take the blood is ejected upward toward the heart, when the muscles relax as we lift our leg in stride, the blood descends caudally due to gravity, that is where the venous valves come into play. They prevent the back-flow of blood. Faulty valves lead to pooling of blood in the veins which overtime dilates them leading to varicose veins.
Anatomy
The lower extremity venous system arises from the inferior vena cava (IVC) which bifurcates into bilateral common iliac veins (CIV) .
Lower Extremity Veins

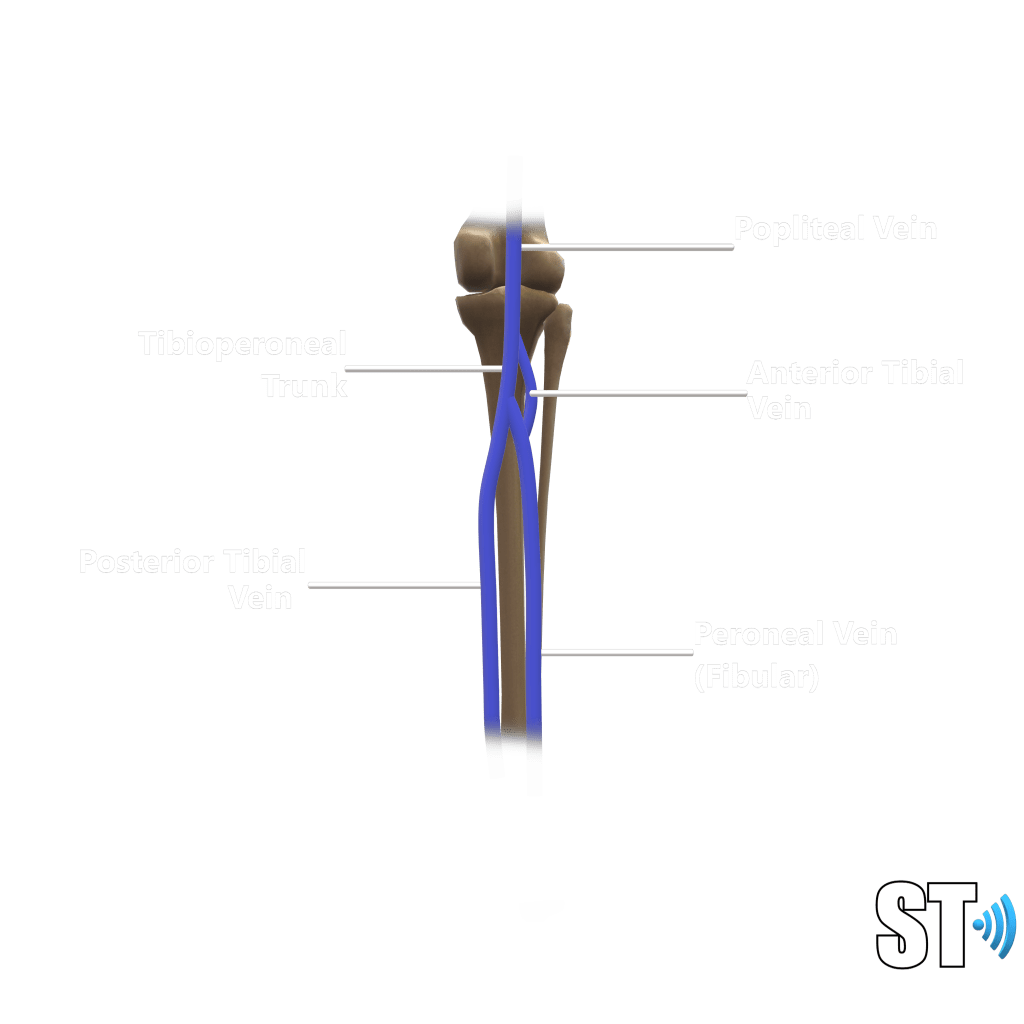
The CIV further branches out into internal iliac vein (IIV) and external iliac vein )EIV.

We follow the EIV which extends caudally into the common femoral vein (CFV) via the inguinal canal where just below we encounter the saphenofemoral junction, (CFV and great saphenous vein).
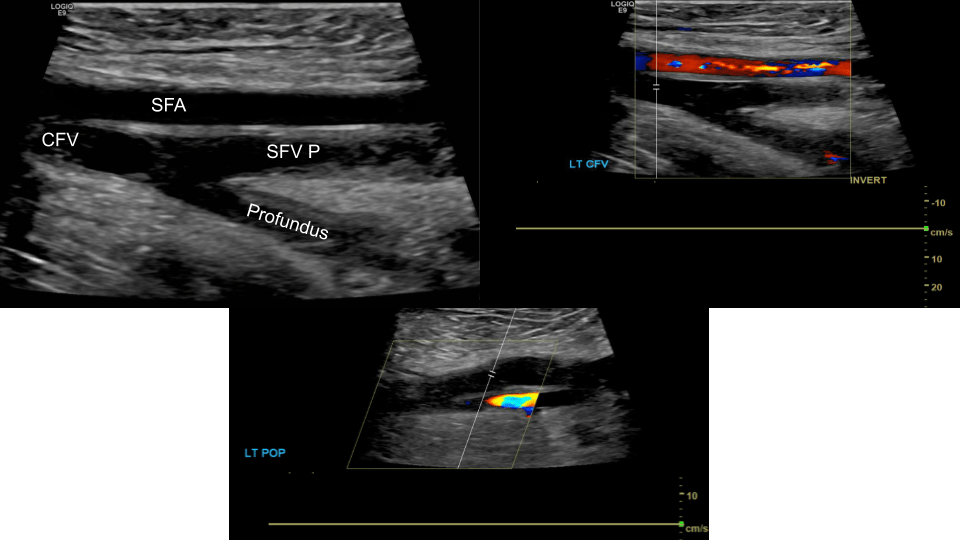
The CFV bifurcates into femoral vein (formerly superficial femoral vein, SFV) and the profundus or deep femoral vein. the SFV courses inferiorly to become the popliteal vein (POP), from the popliteal vein the trio of anterior, posterior tibial and peroneal (fibular) veins arises from the tibio-peroneal trunk.
These form the major veins we evaluate during a lower extremity duplex.
Protocols do vary from institution to institution, as such some places require you to examine from the IVC below, others just from the CFV. The American Institute of Ultrasound in Medicine (AIUM) protocol calls for at the very least inclusion of bilateral EIV’s.
If symptoms are in the calf the soleal and gastrocnemious veins may be monitored as well as the small saphenous vein.
Indications
-Swelling, edema
-pain
-palpable cord (thrombosed superficial vein)
-history of DVT or Pulmonary embolus
-positive laboratory work (d-dimer)
-positive Homans’s sign (calf pain at dorsiflexion of the foot)
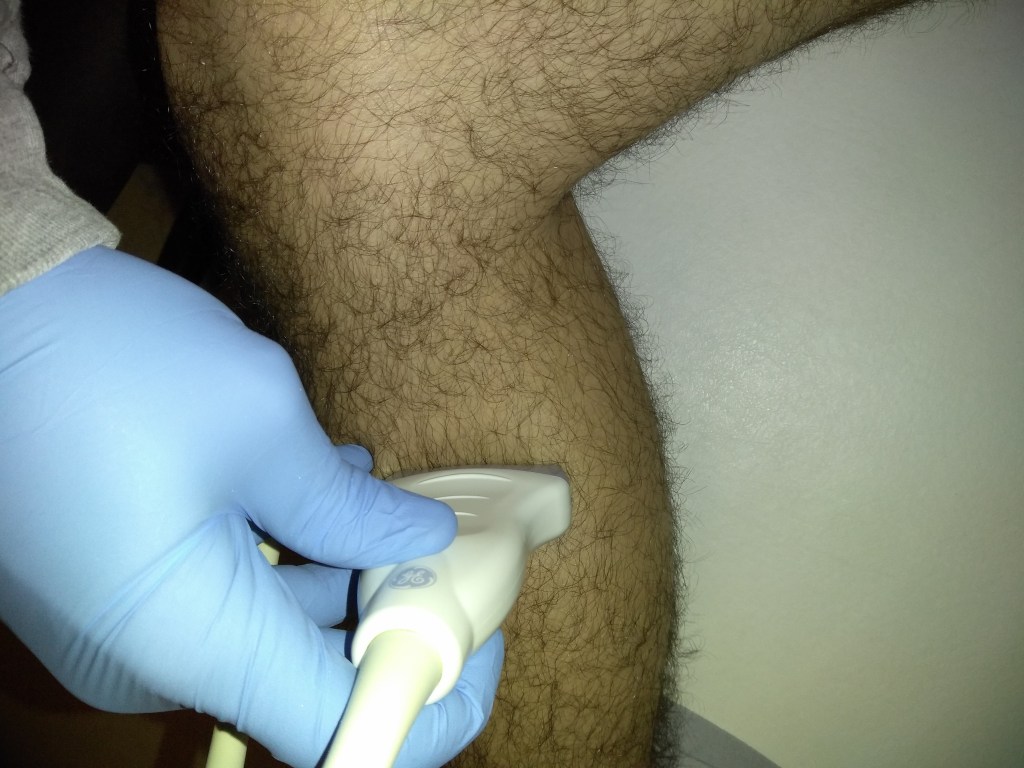
Basic Protocol
Common Femoral Vein: Dual image with compression, grayscale, color doppler, color doppler and pulsed wave doppler
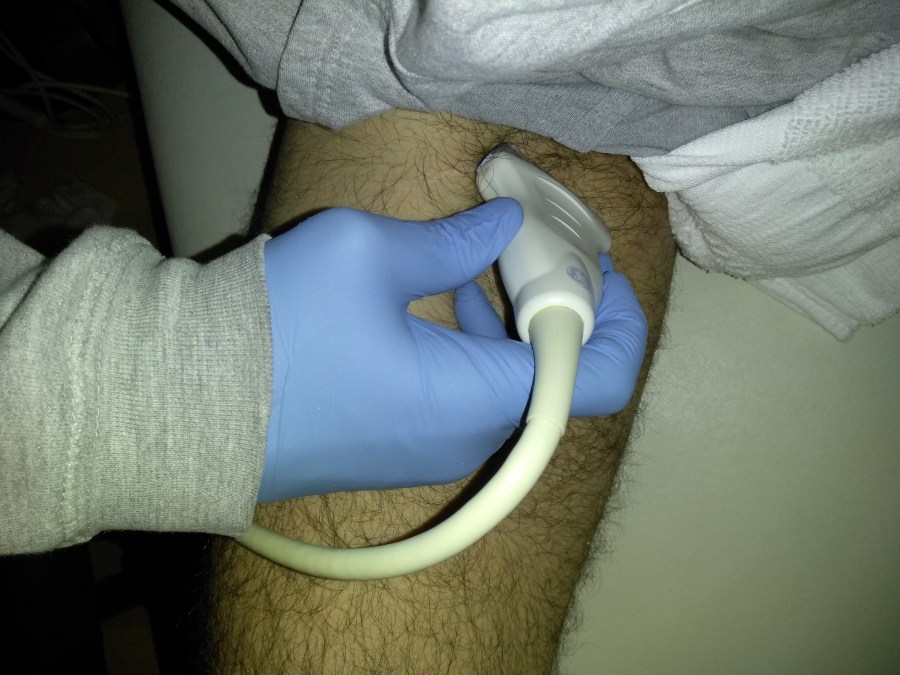
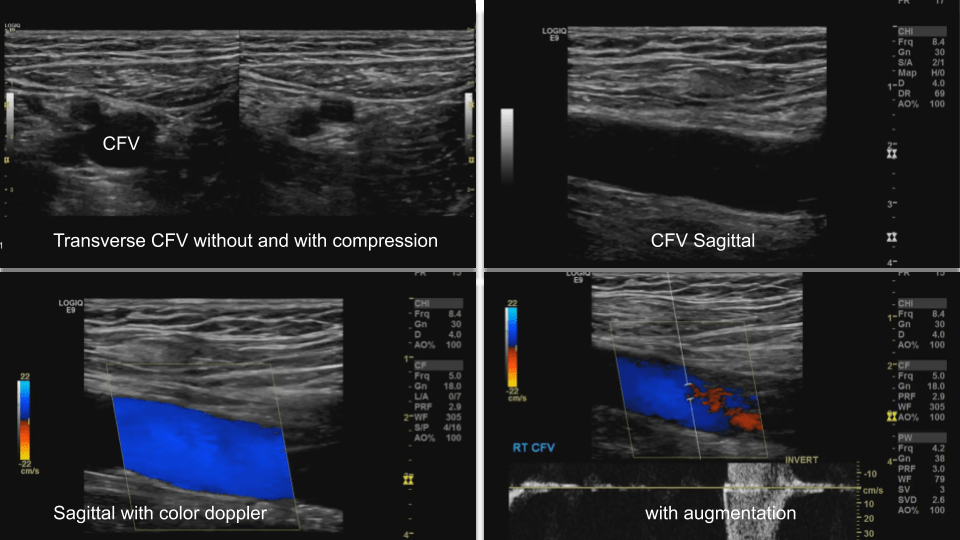
Femoral Vein: Dual image with compression, greyscale, color doppler, color doppler and pulsed wave doppler (scan proximal to distal)
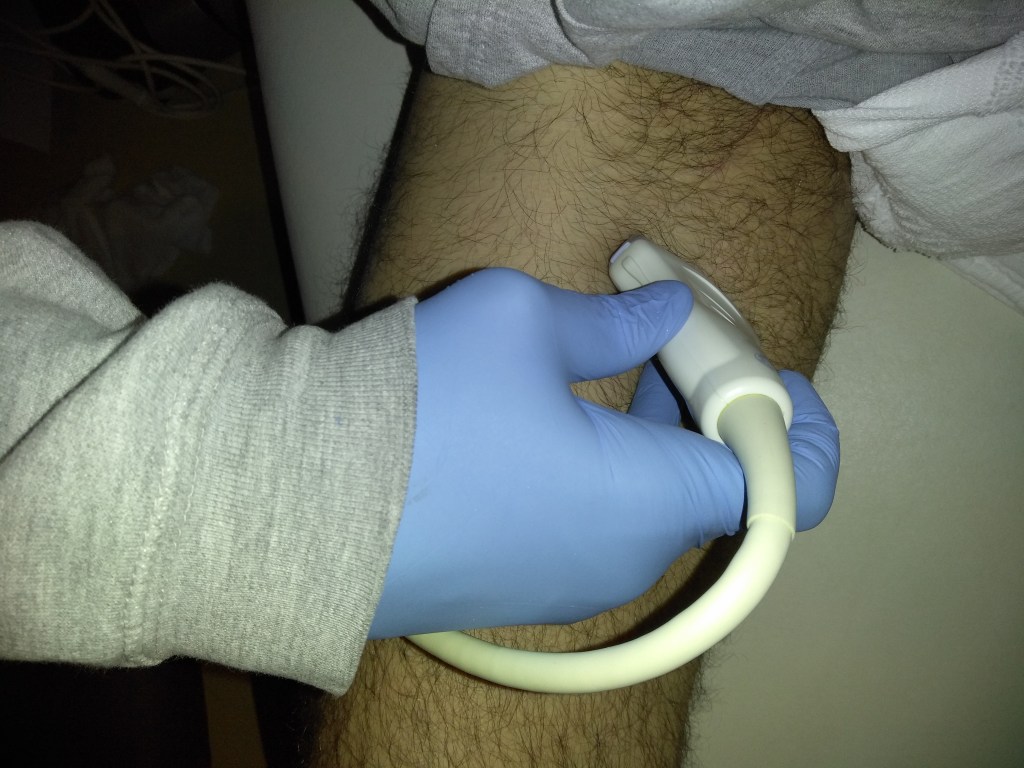
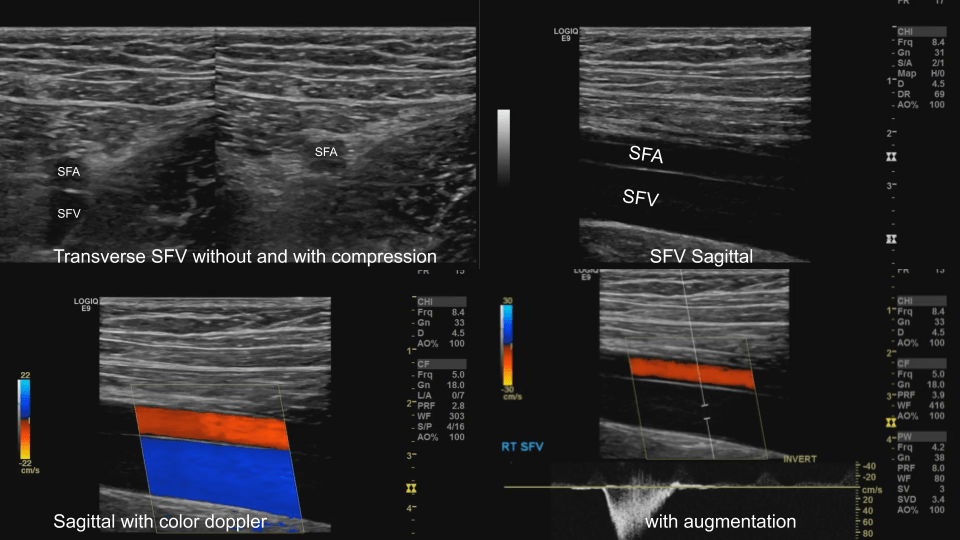
Popliteal Vein: Dual image with compression, greyscale, color doppler, color doppler and pulsed wave doppler
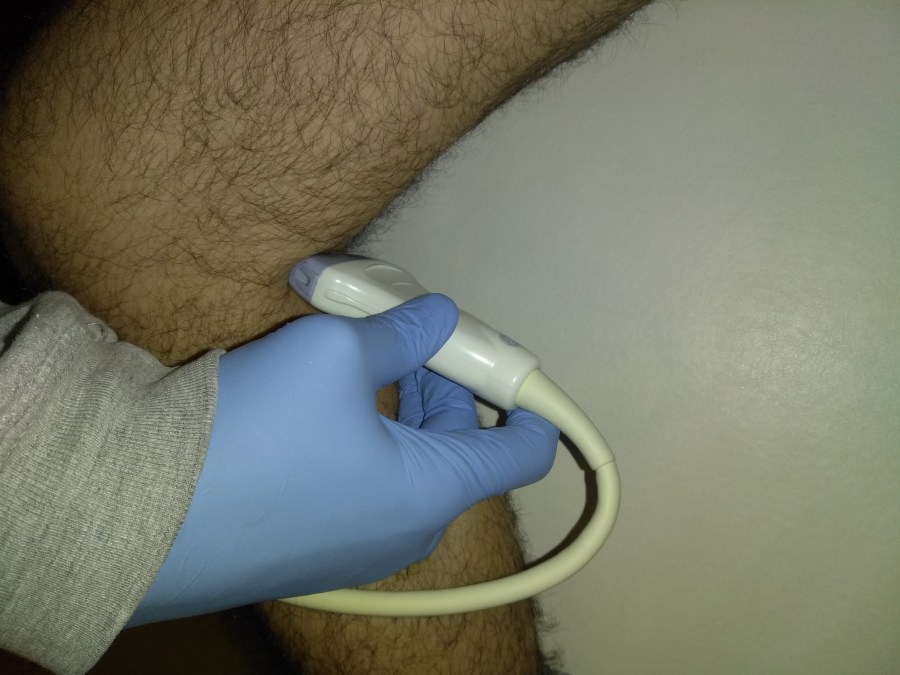
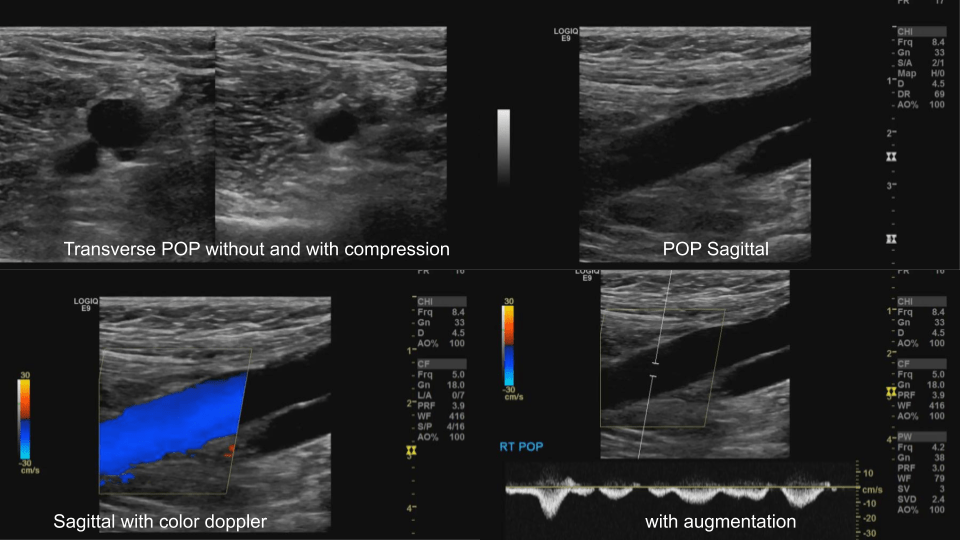
Extra images depending on symptomatology.
Tibio-Peroneal veins
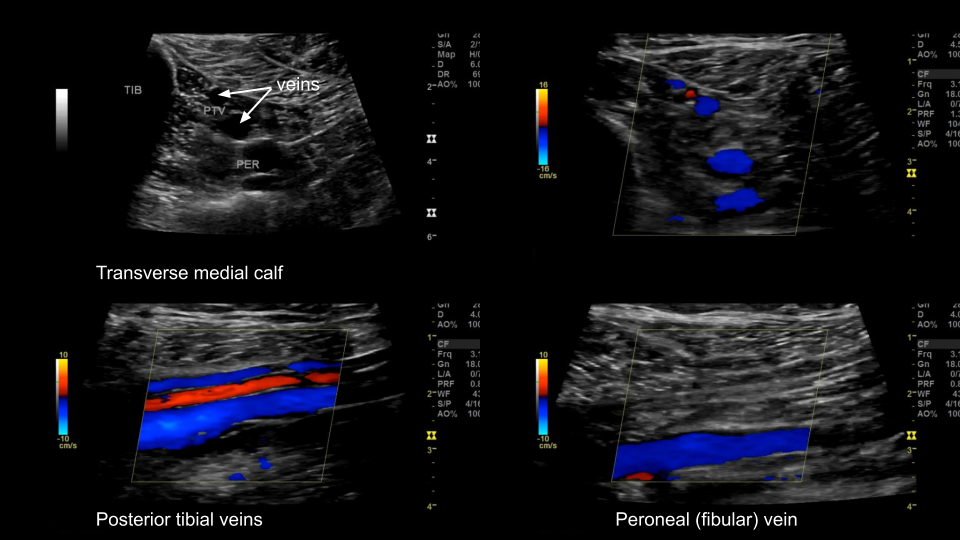
Deep Vein Thrombosis (DVT)
Deep vein thrombosis (DVT) is the development of a thrombus in a deep vein.
Symptoms
- pain
- edema
- redness
- enlarged veins
One of the complications of DVT is the a piece of clot breaking off and lodging in the pulmonary arteries i.e. a pulmonary embolism, which is a life threatening condition.
The most frequent long-term complication is post-thrombotic syndrome, which can cause pain, swelling, a sensation of heaviness, itching, and in severe cases, ulcers.[5] Also, recurrent VTE occurs in about 30% of those in the 10 years following an inital VTE. Another common sequela of DVT is varicose veins from damaged venous valves.
Risk factors
- surgery
- older age
- cancer
- obesity
- history of DVT
- trauma
- immobility (bed ridden)
- hormonal birth control
- pregnancy
- antiphospholipid syndrome
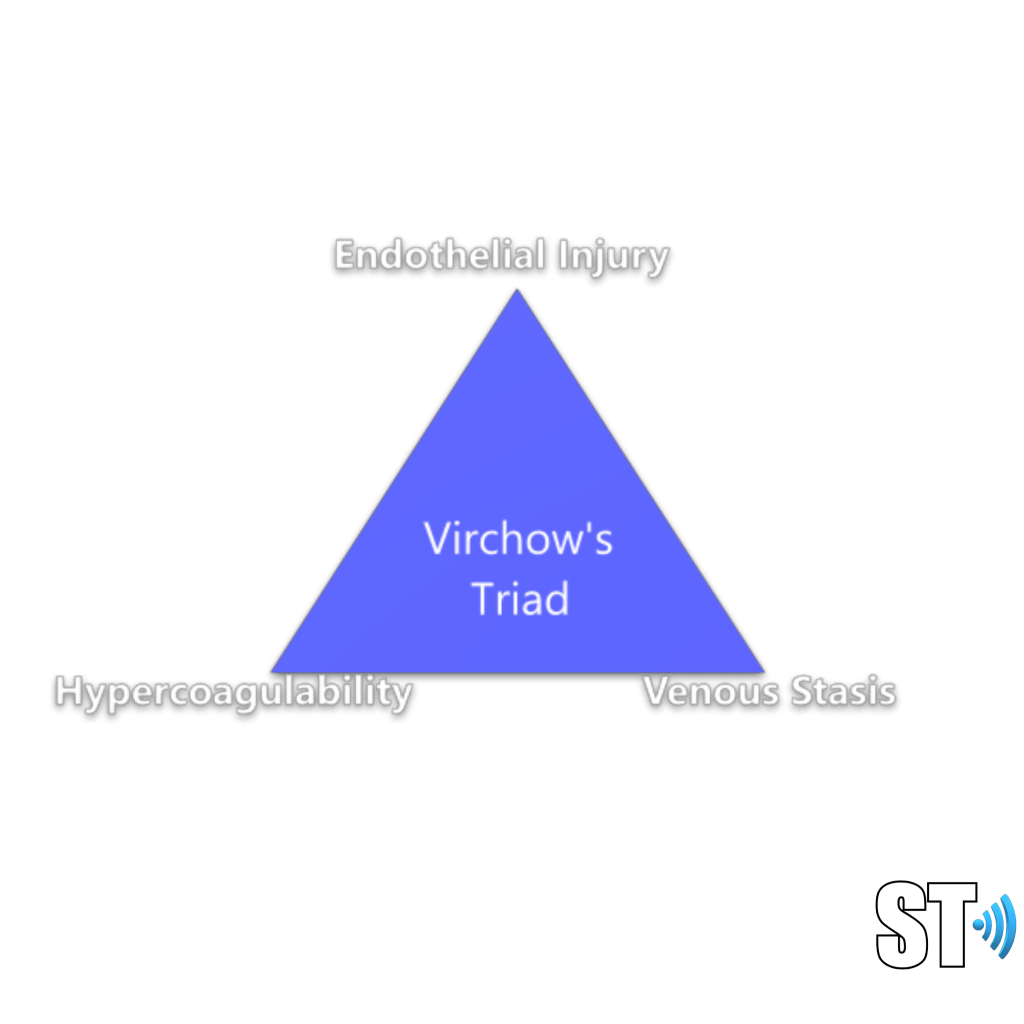
The factors involved in causing DVT are known as Virchow’s triad.
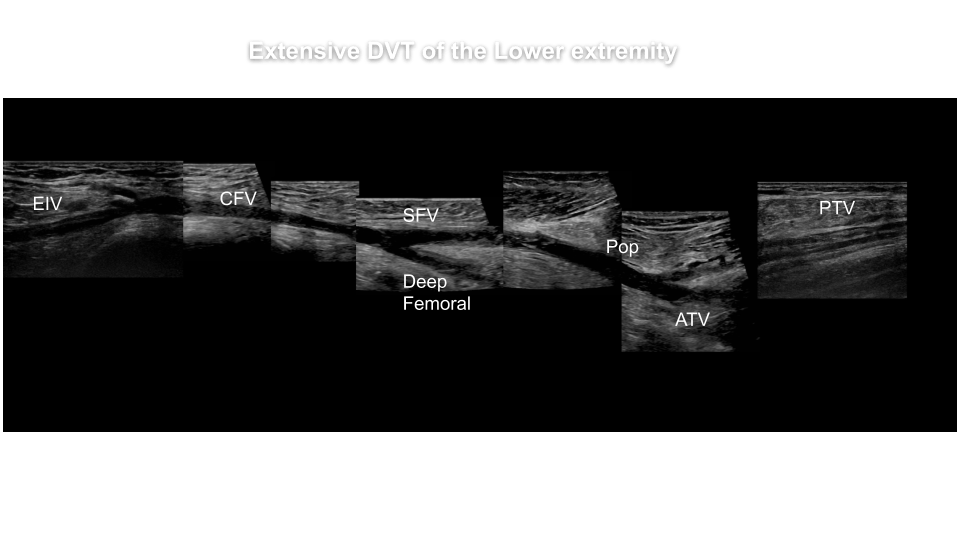


[…] Preform a venous duplex exam protocol, while evaluating for reflux. […]
LikeLike
Is it compatible with any android system or only Iphone
LikeLike
It’s compatible with android and Apple you have to download an app
LikeLike
Your content is super helpful, I’m in ultrasound school thank you Henryyyy
LikeLike